Follow our blog
http://shoulderarthritis.blogspot.com/
On which we try to provide the best and most current information on shoulder arthritis.
Basics of osteoarthritis
Osteoarthritis, or degenerative joint disease (DJD), is a form of arthritis characterized by the loss of joint smoothness and range of motion without major joint inflammation.
Facts and myths
Fact: Low bone density is not associated with osteoarthritis
Bone density is actually HIGHER, rather than LOWER, in osteoarthritis. Low bone density is the telltale sign of osteoporosis, a skeletal disorder characterized by weakened bones due to excessive loss of bone mass.
Osteoarthritis, on the other hand, is characterized by increased bone density and bony growths (osteophytes) in conjunction with articular cartilage degeneration.
Osteoporosis and osteoarthritis are two different diseases with opposite bone density problems.
Fact: Drinking milk cannot prevent osteoarthritis
Milk is an excellent source for calcium which is important for bone formation.
However, a low calcium diet is known to increase one's chance of getting osteoporosis, not osteoarthritis.
Calcium intake is not directly associated with the onset of osteoarthritis. Vitamins A, C and E, the major antioxidants, have been identified as having a potential for protecting cartilage and connective tissue from oxygen radical damage. Vitamin D may also play an important role in osteoarthritis by way of bone mineralization and cell differentiation. Good dietary practices may help protect individuals against osteoarthritis to some extent.
Fact: Osteoarthritis does not cause bone erosion.
Osteoarthritis does not cause bone loss or fractures. On the contrary, it is associated with increased bone density and abnormal growths (osteophytes) due to the deficiency in bone resorption.
Weak, porous bone structures due to low bone density is the signature symptom of osteoporosis, a different and separate disease.
Incidence
Osteoarthritis, or degenerative joint disease (DJD), is the most common type of arthritis, affecting over 20 million people in the United States. DJD probably affects almost every person over age 60 to some degree, but symptoms are often mild.
Some individuals have an inborn tendency to degenerative joint disease because they have changes in the structure of the important protein-building blocks of the articular cartilage which covers the surface of their joints. These seemingly small but significant abnormalities predispose the joint to wear and degeneration. In other cases, joint injuries may contribute to the development of DJD.
Anatomy
In the hip, DJD may produce pain around the groin or in the inner thigh. Some people feel referred pain to the buttocks, the knee or along the side of the thigh. Degenerative joint disease of the hip may cause a limp and may limit range of motion, for example, making it difficult to spread the legs.
Degenerative joint disease of the knees may produce pain and stiffness of the knee associated with a grating or catching sensation in the joint when it is moved. It may make it difficult to walk up and down stairs, and lumps may be noted particularly along the medial (inner side) of the knee. If the pain prevents you from moving or exercising your knee, the large muscles around the knee area will become weaker.
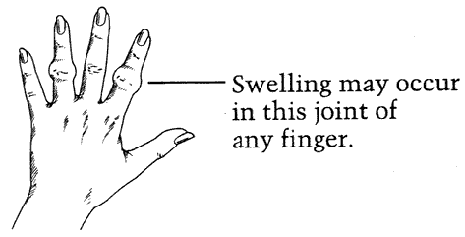
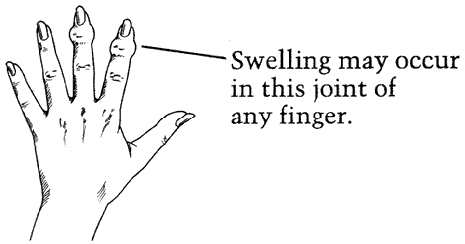
Degenerative joint disease of the fingers may produce bony lumpiness around the joints of the finger and perhaps pain and stiffness of these joints as well. In the fingers: The breakdown of joint tissue in the fingers causes bony growths (spurs) to form in these joints. If spurs occur in the end joints of the fingers, they are called Heberden's nodes. If they occur in the joints in the middle of the fingers, they are called Bouchard's nodes (see figures 1 and 2).
Degenerative joint disease of the feet most commonly affects the large joint at the base of the big toe. Stiffness, lumpiness and pain may be associated. Wearing tight shoes and high heels can make this pain worse.
Degenerative joint disease of the spine may produce stiffness of the back and at times symptoms of pressure on the spinal cord and nerves running through the spine. The latter are particular important to notice and may include numbness or weakness of the arms or legs, difficulty with controlling bowel or bladder, loss of balance and pain radiating out the arms or down the legs.
Bone spurs
Bone spurs are of two basic types. One is the kind that arises near a joint with osteoarthritis or degenerative joint disease. In this situation, the cartilage has been worn through and the bone responds by growing extra bone at the margins of the joint surface. These "spurs" carry the formal name "osteophytes." They are common features of the osteoarthritic shoulder, elbow, hip, knee and ankle. Removing these osteophytes is an important part of joint replacement surgery, but removing them without addressing the underlying arthritis is usually not effective in relieving symptoms.
The second type of bone spur is the kind that occurs when the attachment of ligaments or tendons to bone become calcified. Thus can occur on the bottom of the foot around the Achilles Tendon and in the coroacoacromial ligament of the shoulder. Thus spurs often look impressive on X-rays, but because they are in the substance of the ligaments rarely cause sufficient problems to merit excision.
Symptoms
Osteoarthritis is characterized by clinical symptoms of joint pain and aching, limited range of motion and instability, radiographic evidence of the erosion of the articular cartilage joint space, narrowing sclerosis of the subchondral bone and osteophytes (spurs). Other symptoms include stiffness and roughness on motion; these symptoms are worse after heavy use.
OA pathological changes involve both the cartilage and the bones. Until about 20 years ago, OA was widely assumed to reflect the passive erosion of the bearing surfaces of cartilage in the joints. Degeneration of the articular cartilage was viewed as a normal aging process, much like old tires on a car wearing themselves out after extensive usage. This view is rapidly changing. Degeneration and loss of the articular cartilage in osteoarthritis is explained in terms of the pathophysiologic processes involved in the metabolism of cartilage, rather than the inevitable mechanical wear and tear due to aging.
If degenerative joint disease is related to abnormalities of articular cartilage, it may involve many of the joints of the body. On the other hand, if the degenerative joint disease is caused by an injury, only one joint may be involved. The hips, knees, spine and shoulders are most commonly involved. This condition may also affect some finger joints the joint at the base of the thumb and the joint at the base of the big toe.
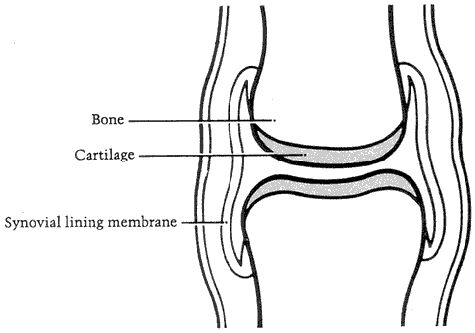
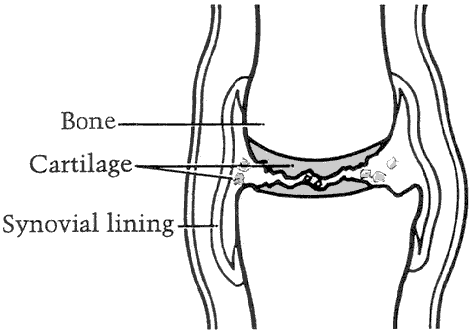
The typical joint changes in osteoarthritis can be seen by comparing a healthy joint with a joint with osteoarthritis (see figures 3 and 4). In osteoarthritis, the normally smooth cartilage surface softens and becomes pitted and frayed. As the cartilage breaks down, the joint may lose its normal shape. The bone ends thicken and form bony growths or spurs where the ligaments and capsule attach to the bone.
Stiffness and joint deformity usually progress slowly without general body symptoms. By contrast, rheumatoid arthritis (RA) usually begins earlier, often developing more suddenly. RA usually affects same joint on both sides of body (e.g. both knees) causing redness, warmth and swelling of many joints. RA is often accompanied by a general feeling of sickness, fatigue, weight loss and fever.
Causes
It is difficult to determine the initial event that leads to the onset of OA. Nonetheless, all hypotheses associate the OA changes to the mechanical overloading of the joints.
"Wear and tear" is a widely accepted explanation of the cause of OA. It should be noted that OA is the result of an interlocking pathophysiologic malfunction of cartilage and bone metabolism. Interpreting "wear and tear" of the joints in OA from a biomechanic perspective allows patients to understand how OA differs from age-associated degeneration and overuse of the joints. There are ways to reduce the OA "wear and tear" effects which include weight control, muscle strengthening exercises and increased proprioception accuracy.
It is a common view that OA begins as a fibrillation of articular cartilage, a focal fine roughening of the surface of articular cartilage, that eventually leads to secondary remodeling of the bony components of the joint. Remodeling refers to the resorption and formation of bone tissues under the influence of mechanical loading history on the joints.
An alternative hypothesis suggests that OA originates from the stiffness of subchondral bone. Normally, it is the bone, not the cartilage, that absorbs most of the impact forces on the extremities. This "stiff bone" hypothesis suggests that mechanical overloading on the joints may result in microfractures in subchondral bones underlying the articular cartilage. The repair of the fractures leads to a net local increase of the stiffness of the bone. The "stiff bone" provides less cushion for the overlying cartilage and thus forces the cartilage to absorb a greater share of the impact energy. The repartition of forces eventually leads to the degeneration of the articular cartilage. The relationship between cartilaginous and bony changes in OA is very complex and intertwined.
A third and less established hypothesis associates proprioceptive impairment with knee OA. Proprioception refers to the conscious and unconscious perception of joint position and movement. Accurate proprioception is critical to maintain joint stability under dynamic conditions. Joint stability is important to prevent the wear and tear from mechanical forces on the extremities.
Osteoarthritis Photo Gallery
Treatment
The effects of degenerative joint disease can often be controlled by a few basic measures such as diet, exercise, medication and surgery.
Diet
If you have DJD, your diet should optimize your body weight, so that the joints do not bear large loads which would cause them to wear more quickly.
Exercise and therapy
Joints in a person with DJD should be protected from rough use, particularly those involving sudden impacts. Canes or walkers may help protect the hip and knee and prevent limping.
Joint range of motion strength and stability should be maintained by regular gentle exercise.
Medications
If you have DJD, your doctor may prescribe Nonsteroidal anti-inflammatory drugs (NSAIDs).
Surgery
Surgical treatment for DJD may include removing joint spurs, realigning the joint, fusion of the joint and joint replacement. In the past several years, these operations have become very effective and many people have benefited from joint repair or replacement.
Condition research
There has been much progress in arthritis research. New information regarding the development structure and degradation of joint cartilage is becoming available. Scientists are studying the complex ways joints move and fit together and how joints respond to many different stresses and strains. They also are continuing to improve ways to avoid further damage to the bones and tissue. Researchers have also identified a gene that may be linked to the faulty development of cartilage, thus leading to the development of osteoarthritis or other conditions. Finally, surgeons are devising better procedures for restoring comfort and function to joints affected by arthritis.
Credits
Some of this material may also be available in an Arthritis Foundation brochure.
Adapted from a pamphlet originally prepared for the Arthritis Foundation. This material is protected by copyright.