Last updated: Tuesday, January 25, 2005
About rotator cuff failure
The young healthy cuff is highly resistant to disruption or degeneration. Because of the change in cuff strength with age (see figures 1 and 2) full thickness cuff lesions are most unusual under the age of 40. When cuff lesions occur in the younger age group they may be only partial thickness or they may include the avulsion of bone from the tuberosity (see figure 3). Disuse and scarring of the partial thickness lesion may lead to stiffness limiting the range of elevation cross-body adduction and internal rotation.
With increasing age and disuse less force is required to tear the cuff. Often the acute symptoms from progression of the cuff defect are dismissed as "tendinitis" or "bursitis." Once these transient symptoms resolve the shoulder becomes asymptomatic except for a relatively imperceptible increment in weakness. Thus we often encounter patients with large cuff defects and minimal symptoms. If these shoulders remain stable with the humeral head centered in the glenoid they can demonstrate an astounding degree of function. Bilateral degenerative cuff defects are common. In one of our studies we found that 55 percent of patients presenting with a symptomatic cuff tear on one side also had a tear on the opposite side.
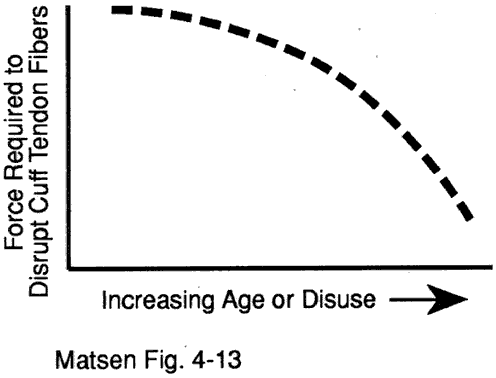
Figure 1 -
Cuff strength changes with age
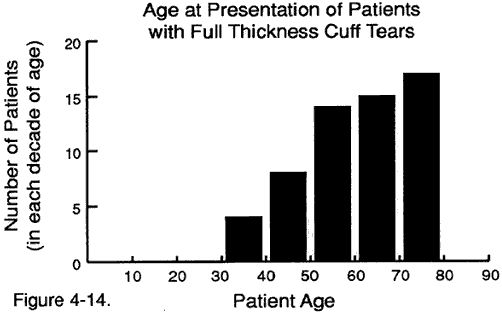
Figure 2 -
Age at presentation of patients
with full thickness rotator cuff tears
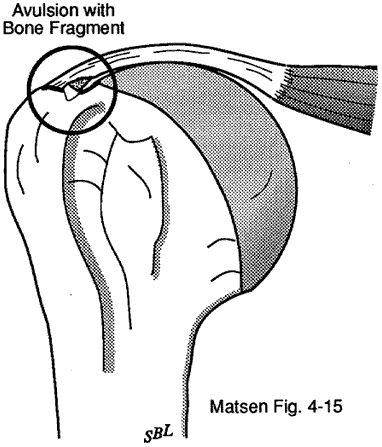
Figure 3 -
Avulsion of bone from the tuberosity
Progression of cuff failure
Cuff failure may progress as major episodes of tendon tearing or as creeping tears involving relatively few fibers at a time with thinning of the cuff tendon.
Typical progression
Degenerative lesions of the cuff typically start at the deep surface of the anterior insertion of the supraspinatus near the long head of the biceps. Once these lesions begin it is difficult for them to heal because of the hostile environment the compromised vascularity the large loads and the large deformations that the healing tissue must endure. Failure of one fiber or of groups of fibers places greater loads on the adjacent fibers favoring their failure (the "zipper" phenomenon). When a tendon fiber fails the muscle fiber to which it attaches produces retraction away from the site of disruption increasing the gap needing to be closed. This retraction also places tension on the local vasculature leading to limitation of tendon blood flow in the area where healing is needed.
Rotator cuff tendon defects are subject to the effects of synovial fluid on both their articular and bursal sides; the fluid and its enzymes may remove the fibrin clot necessary for healing of the cuff lesion. In the absence of repair the degenerative process tends to continue through the substance of the supraspinatus tendon to produce a full thickness defect in the anterior supraspinatus tendon. This full thickness defect tends to concentrate loads at its margin facilitating additional fiber failure with smaller loads than those which produced the initial defect.
Once a supraspinatus defect is established it typically propagates posteriorly through the remainder of the supraspinatus then into the infraspinatus and teres minor. Further propagation of the cuff defect crosses the bicipital groove to involve the subscapularis starting at the top of the lesser tuberosity and extending inferiorly. As the defect extends across the bicipital groove it may be associated with rupture of the transverse humeral ligament and destabilization of the long head tendon of the biceps.
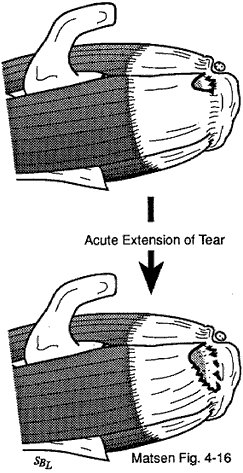
Figure 4 -
Major episodes of tendon tearing
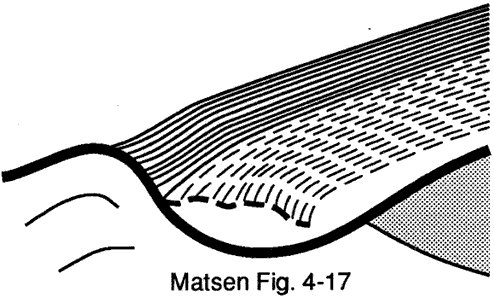
Figure 5 - Creeping tears
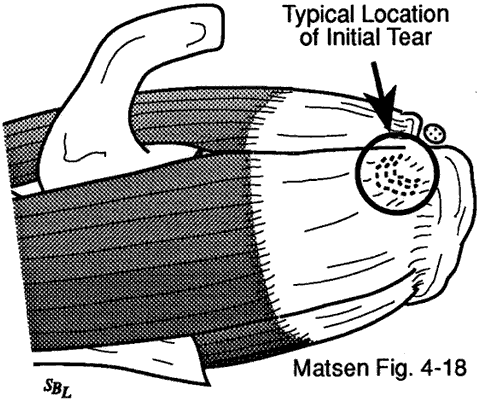
Figure 6 -
Degenerative lesions of the cuff
generally start at the deep surface
of the anterior insertion
of the supraspinatus near
the long head of the biceps
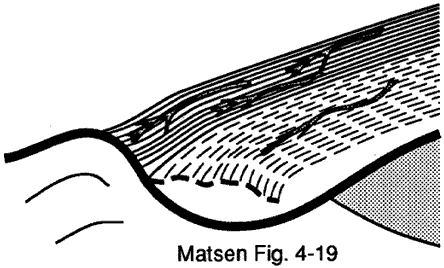
Figure 7 -
Limitation of tendon blood flow
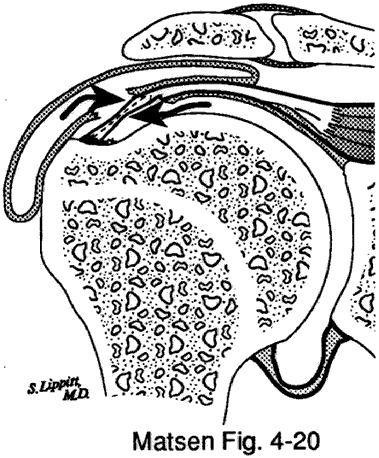
Figure 8 - Articular and bursal sides
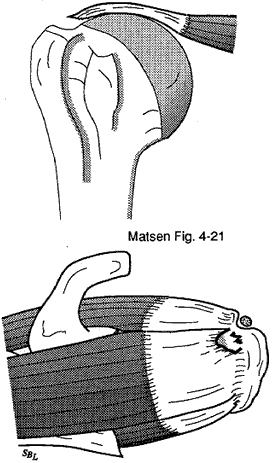
Figure 9 -
Full thickness defect

Figure 10 - Additional fiber failure
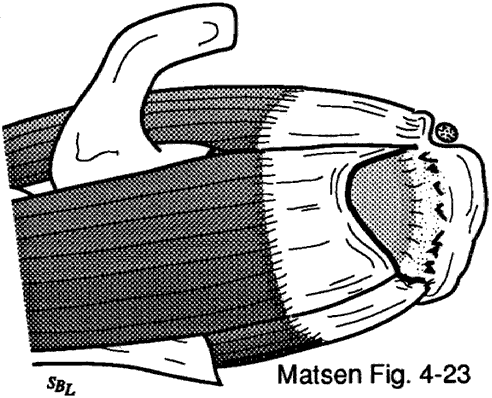
Figure 11 -
Infraspinatus and teres minor
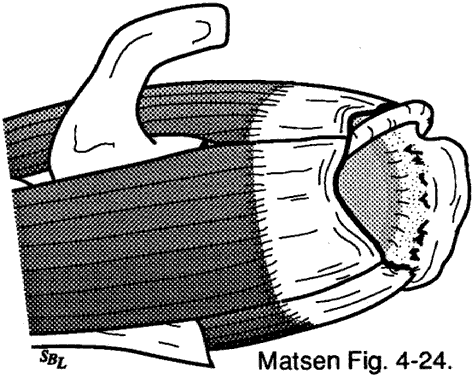
Figure 12 -
Destabilization of the
long head tendon of the biceps
Effects of cuff failure
The concavity compression mechanism is compromised by cuff disease. Beginning with the early stages of cuff fiber failure the compression of the humeral head becomes less effective in resisting the upward pull of the deltoid. Partial thickness cuff tears cause pain on muscle contraction similar to that seen with other partial tendon injuries (such as those of the Achilles tendon or extensor carpi radialis brevis). This pain produces reflex inhibition of the muscle action. In turn this reflex inhibition along with the absolute loss of strength from fiber detachment makes the muscle less effective in balance and stability. The weakened cuff function allows the humeral head to rise under the pull of the deltoid squeezing the cuff between the head and the coracoacromial arch. Under these circumstances abrasion occurs with humeroscapular motion further contributing to cuff degeneration. Degenerative traction spurs develop in the coracoacromial ligament which is loaded by pressure from the humeral head (analogous to the calcaneal traction spur that occurs with chronic strains of the plantar fascia). Upward displacement of the head also wears on the upper glenoid lip and labrum reducing their contributions to the effective depth of the upper glenoid and to glenohumeral stability from concavity compression.
Further deterioration of the cuff allows the tendons to slide down below the center of the humeral head producing a "boutonniere" deformity. The cuff tendons become head elevators rather than head compressors. Once the full thickness of the cuff has failed abrasion of the humeral articular cartilage against the coracoacromial arch may lead to a secondary degenerative joint disease known as cuff tear arthropathy.
The progression from partial thickness tear toward cuff tear arthropathy can take place as a subtle and even subclinical degenerative process with a few fibers giving way at a time. It can also progress as a series of episodes interpreted as "tendinitis bursitis or impingement syndrome." A more significant injury can produce an acute extension of the defect. It is important to note that cuff defects arising with minimal or no injury suggest that the cuff tissue is of poor quality and thus is more likely to fail again after surgical repair. By contrast acute tears resulting from major injuries are more likely to involve robust tissue that is more amenable to a durable repair.
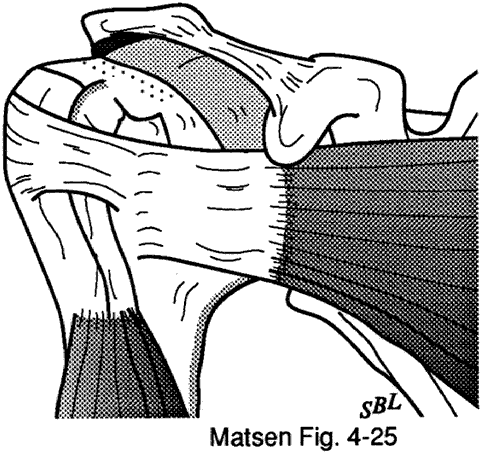
Figure 13 - "Boutonniere" deformity
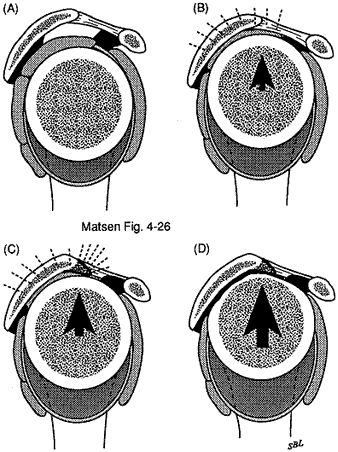
Figure 14 - Cuff tear arthropathy
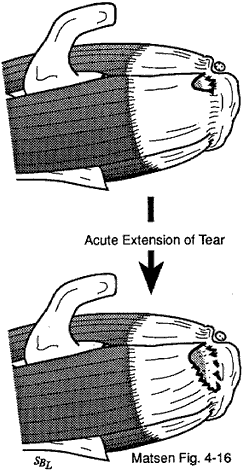
Figure 15 - Acute extension of the defect
The disuse of torn tendon leads to scarring and atrophy of tendon and muscle. Loss of cuff material from the degenerative process limits what is available for repair. Local injections of steroids may further compromise the healing potential of failed cuff fibers. Once the humeral head has started to subluxate superiorly increased stretching loads are placed on the residual tendons tending to exacerbate the cuff defect. Long-standing superior subluxation leads to erosion of the upper glenoid lip favoring continued superior subluxation even after cuff repair. Once the process of superior subluxation is established stabilization of the humeral head in its normal position is difficult even if a cuff repair is achieved.
In summary
Rotator cuff defects are common causes of shoulder weakness. Usually cuff tears are associated with degenerative changes which make the tissue susceptible to failure with low applied loads especially those applied eccentrically. Alternatively cuff tears can occur in stronger cuff tissue but these injuries require the application of much greater loads. Cuff defects produce weakness of elevation and external rotation as well as a possible loss of stability of the humerus against upward displacing loads from the deltoid. Shoulders may be comfortable and able to carry out certain functions in the presence of significant cuff defects. Rotator cuff surgery can restore the strength of the shoulder if the cuff tissue is of sufficient quantity and quality. To minimize the risk of retear a substantial period of minimal loading needs to follow cuff repair surgery. Returning to heavy work after a cuff repair risks the integrity of the repair. Preservation of deltoid function is essential in rotator cuff surgery. If the function of both the cuff and deltoid are lost glenohumeral arthrodesis may represent the only surgical option for salvage.