Ream and Run non-prosthetic glenoid arthroplasty for shoulder arthritis: Regenerative cementless surgery designed for individuals desiring higher levels of activity than recommended for traditional total joint replacement
Last updated: December 12, 2013
Edited by:
Follow our blog
http://shoulderarthritis.blogspot.com/
On which we try to provide the best and most current information on shoulder arthritis.
To read more about Shoulder Arthritis, please visit our online Shoulder Arthritis Book.
Contact
If you have questions regarding the ream and run procedure, feel free to email Frederick A. Matsen III, M.D. at matsen@uw.edu.
Overview
Non-prosthetic glenoid arthroplasty sometimes called the "ream and run" procedure is a surgical treatment that can help relieve the pain from severe arthritis of the shoulder. Unlike conventional "metal on plastic" total shoulder replacement (total shoulder arthroplasty) the "ream and run" approach may allow active patients to remain involved in fitness recreational and vocational pursuits that would risk premature failure if traditional total shoulder arthroplasty were to be performed.
The shoulder is a ball and socket joint that allows the arm to be placed in an incredibly wide range of positions during every day activities. The ball is formed by the head of the humerus (arm bone) and the socket is formed by the scapula (shoulder blade). The socket is also referred to as the glenoid. The surfaces of the ball and socket are formed by cartilage a tissue that allows joints to glide in a smooth and frictionless way.
Arthritis of the shoulder is a condition in which the cartilage on the humeral head and glenoid deteriorates. As this process becomes more advanced the joint surfaces become rough and areas of bone may be exposed. Figure 1 shows the surface of a humeral head destroyed by arthritis. Motion of the arthritic joint causes the surfaces to grate rather than glide. Progressive joint destruction makes the shoulder stiff painful and unable to carry out its normal functions.
When pain and loss of function become disabling enough for a patient to consider treatment joint replacement surgery is the most reliable solution for shoulder arthritis. The goals of shoulder replacement are to restore comfort and function to the joint by removing scar tissue balancing muscles and replacing the destroyed joint surfaces with artificial ones.
While total shoulder replacement surgery has proven to be a successful treatment for advanced shoulder arthritis the artificial components are not designed to withstand some of the demands that active individuals expect to place on them once comfort and function have been restored. As more and more people continue participation in sports and other recreational activities into their older years they may slowly begin to exceed the limits of what the artificial components can tolerate.
This is particularly true for the plastic socket that is prone to wear out loosen or even break in very active individuals. Patients who intend to return to activities that place physical demands on the shoulder replacement (such as golf tennis skiing weightlifting etc.) may therefore be at risk for eventual failure of the artificial shoulder socket. When failure of the socket occurs patients typically experience a dramatic decrease in their comfort and function.
Therefore a conventional total shoulder replacement which resurfaces the arthritic socket with a plastic component may not be the best option in terms of preserving comfort and function in very active patients. In these patients an alternative that removes the destroyed cartilage and provides a smooth and stable surface without insertion of the plastic socket may be more sensible.
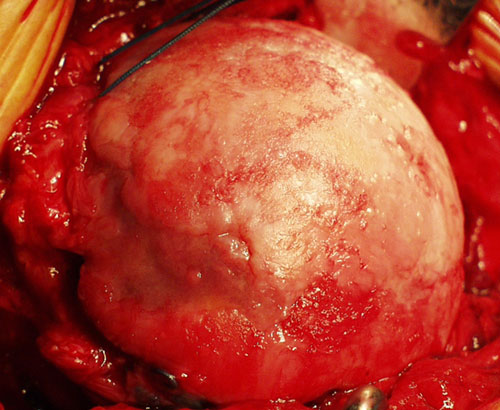
Humeral head that has
been damaged by arthritis.
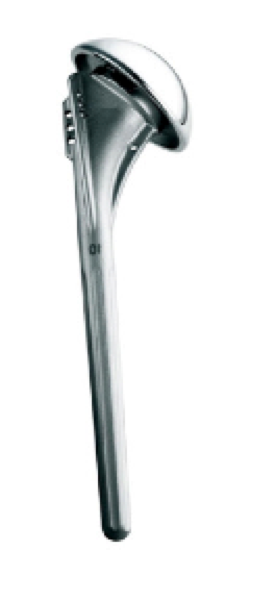
Humeral component
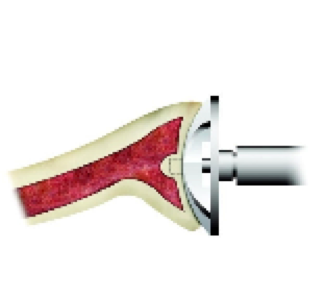
Reaming the glenoid.
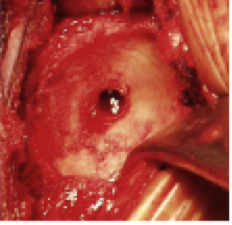
The reamed glenoid socket.
This alternative is referred to as shoulder hemiarthroplasty with non-prosthetic glenoid arthroplasty or a ream and run procedure. It uses a prosthetic humeral ball (which is made of metal) (see figure 2). The humeral ball is fixed to the humerus (arm bone) by attachment to a stem that rests securely inside the hollow canal of the bone. The glenoid socket is reamed (Figure 3) to a smooth convexity (Figure 4).
Because the socket side of the joint is reshaped and the ball side replaced the rough arthritic surfaces are eliminated from both sides of the shoulder joint. By avoiding the use of a plastic socket non-prosthetic glenoid arthroplasty removes the risk of loosening or wear of the polyethylene component Because problems with the metal ball are very rare this procedure should improve the longevity of comfort and function in patients who might otherwise experience earlier problems related to socket loosening or wear.
This procedure has proven successful in restoring comfort and a high level of shoulder function in patients with severe shoulder arthritis. The recovery of comfort may take longer than with conventional total shoulder arthroplasty however. Like a conventional shoulder replacement operation it is a highly technical procedure and is best performed by a surgical team who performs this surgery often. Such a team can maximize the benefit and minimize the risks. The two-hour procedure is performed under general anesthesia.
Shoulder motion is started immediately after the procedure. Patients learn to do their own physical therapy and are usually discharged three days after surgery if they are comfortable and have a good range of passive motion. The recovery of strength and function may continue for up to a year after surgery.
Click here to see the ream and run essentials
5 months after "Ream and Run" surgery


ream and run up on his slalom ski
that had been put away for 7 years"












10 surgery questions for your surgeon before having surgery
Symptoms & Diagnosis
Characteristics of arthritis of the shoulder
Arthritis of the shoulder is a condition in which the cartilage normally covering the joint surfaces is lost.
Individuals with shoulder arthritis usually notice pain stiffness and loss of the ability to use the shoulder for their usual activities. Commonly they have difficulty sleeping on the affected shoulder and limited range of motion. Some people with arthritis notice a grinding feeling when the shoulder is moved. Shoulder arthritis usually gets worse over time but the rate of this progression varies widely.
Types
Shoulder arthritis may be of several types including osteoarthritis (or degenerative joint disease), rheumatoid arthritis, arthritis after injury (traumatic arthritis), arthritis after previous surgery (for example capsulorrhaphy arthropathy), chondrolysis, dysplasia, and arthritis associated with rotator cuff disease (known as cuff tear arthropathy). Arthritis may also follow infection; this is known as septic arthritis. If the ball of the shoulder joint (humeral head) dies from lack of circulation a condition known as avascular necrosis (or osteonecrosis) of the shoulder may result.
Similar conditions
Shoulder arthritis must be distinguished from rotator cuff disease frozen shoulder and neck arthritis each of which may produce similar symptoms. Rotator cuff tears usually cause pain and weakness but stiffness is less common. Frozen shoulder is characterized by shoulder stiffness but the X-rays are usually normal. Neck arthritis may cause shoulder pain and weakness that is worse when the head is held in certain positions.
Incidence and risk factors
Although not as common as rotator cuff disease shoulder arthritis is among the most prevalent causes of shoulder pain and loss of function. Arthritis of the shoulder joint is less common than arthritis of the hip or knee. Individuals with arthritis in one joint are more likely to get it in another joint.
Diagnosis
A physician diagnoses shoulder arthritis by reviewing the patient's history performing a thorough physical examination of the joint and taking the proper X-rays. The examination of an arthritic shoulder reveals stiffness and roughness of the joint.
X-rays of the shoulder reveal the contour of the joint surfaces and the status of the cartilage space between them. X-rays of an arthritic shoulder usually show a narrowing of the space between the ball and socket--often to the point that bone is touching bone. The left side of figure 5 shows bone spurs at the bottom of the joint. The right side of figure 5 shows that the ball is not centered and has worn down the back part of the socket. These findings indicate that the normal cartilage has been destroyed. X-rays do not show the soft tissues such as scar tissue that may also be limiting joint motion.
It is essential that the shoulder surgeon establish the diagnosis of arthritis before shoulder joint replacement is considered.
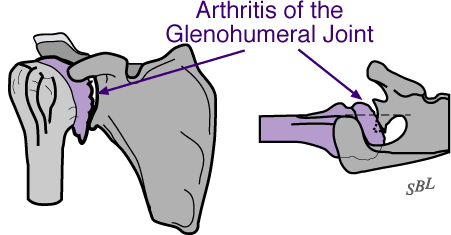
The figure on the left shows bone spurs
at the bottom of the joint. The figure on the right
shows that the ball is not centered
and has worn down the back part of the socket.
Treatments
Medications
Medications may be helpful in managing arthritis. In the case of rheumatoid arthritis specific drugs may treat the inflammation that destroys the cartilage. Some of these medications are administered by injection and others by mouth. Some individuals take anti-arthritic medications for their entire lives. These medications can be quite helpful but there may be side effects. These medications should be taken under the close supervision of a rheumatologist or other physician experienced in their use. In other types of arthritis anti-inflammatory drugs may lessen the pain but do not change the course of the condition. It is important that the patient be aware of the possible side effects of these medications including stomach irritation kidney problems and bleeding. Injections of steroids (cortisone) or lubricants (such as hyaluronic acid) into the shoulder have not been demonstrated to have lasting benefit and carry some risk of infection.
For each medication patients should learn:
- the risks
- possible interactions with other drugs
- the recommended dosage and
- the cost.
Exercises
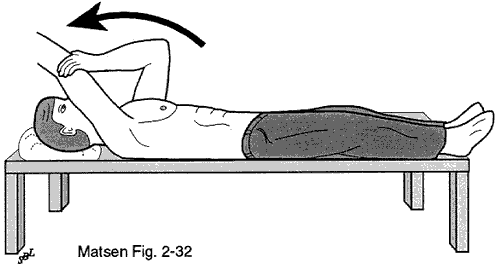
If exercises are not too painful they may be helpful in maintaining the flexibility and strength of joints with arthritis. In most cases these exercises can be done in the patient's home with minimal equipment. Shoulder exercises are best performed gently several times a day on an ongoing basis. Often the exercises will help during the earlier phases of the condition. The exercises are not dangerous if they are performed gently. The diagrams show two examples of these exercises.
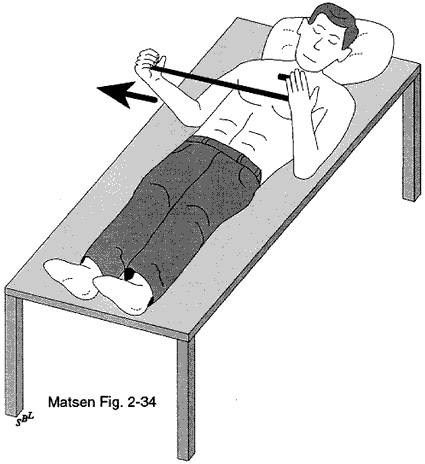
Figure 6 shows a patient using the left arm to help lift the stiff right shoulder in a forward direction. Figure 7 shows a patient using the left arm to gently stretch the stiff right arm in external rotation using a yardstick.
Sometimes other types of therapy are used by physical therapists. Patients should learn the possible risks of these approaches as well as their costs and anticipated effectiveness.
Possible benefits of non-prosthetic glenoid arthroplasty
With proper rehabilitation shoulder hemiarthroplasty with non-prosthetic glenoid arthroplasty restores lost function to arthritic shoulder joints. By removing the damaged joint surfaces this procedure allows the shoulder to move in a smooth and stable manner. In experienced hands this procedure can also address the restricting scar tissue that frequently accompanies arthritis and contributes to pain and stiffness.
Both total shoulder replacement surgery and non-prosthetic glenoid arthroplasty can improve the mechanics of the shoulder but cannot make the joint as good as it was before the onset of arthritis. In many cases the tendons and muscles around the shoulder have been weakened from prolonged disuse before the operation. It can often take months of gentle exercises before the shoulder achieves maximum improvement.
The effectiveness of the procedure depends on the health and motivation of the patient the condition of the shoulder and the expertise of the surgeon. Strict adherence to the rehabilitation program maximizes the chances of a good result from non-prosthetic glenoid arthroplasty. Maintaining general health fitness and nutrition as well as abstinence from cigarette smoking all improve the chances of success. The greatest improvements are in the ability of the patient to sleep to perform activities of daily living and to perform non-contact recreational activities.
Who should consider non-prosthetic glenoid arthroplasty?
Joint replacement surgery is considered when:
- the arthritis is a major problem for the patient
- the patient is sufficiently healthy to undergo the procedure
- the patient understands and accepts the risks and alternatives
- there is sufficient bone and tendon to permit the surgery and
- the surgeon is experienced in shoulder replacement surgery.
What happens without surgery?
The natural history of arthritis is that it usually continues to progress over time. The rate of progression varies between individuals and is unpredictable. Sometimes the pain and stiffness from shoulder arthritis will stabilize at a level that is acceptable and manageable to the patient. In general this surgery is elective and can be performed whenever the patient decides that the arthritis has become disabling enough to warrant treatment. Delaying surgery typically does not compromise the success of surgery in the future. However in cases of rheumatoid arthritis excessive delay may result in loss of the tendon and bone making the surgery more difficult for the patient and for the surgeon.
Surgical options
Several types of shoulder arthroplasty are used to manage arthritis. In total shoulder arthroplasty the surfaces of both the humeral head (ball) and the glenoid (socket) are resurfaced with metal and plastic implants. In shoulder hemiarthroplasty a prosthesis is used only on the humeral side of the joint. Because the humeral component can usually be secured by a press fit most humeral replacement surgery does not require bone cement. As a result the risk of cement failure is eliminated.
The decision about which type of shoulder replacement will maximize benefit and minimize risk depends on several factors. These include the location and severity of the arthritis the age of the patient and the level of physical demand the patient expects to exert on the replaced shoulder. When advanced arthritis has destroyed both the ball and socket then both sides of the joint must be addressed.
As with joint replacement procedures in other parts of the body the plastic components used in the replacement do not last forever. Much like the brakes of a car wear out with use the plastic socket used in total shoulder replacement surgery tends to wear with time. The process can take the form of flattening loosening or breaking. In each case the socket is no longer able to provide a smooth and stable foundation for the ball. Patients will often note that their comfort and function decline as the socket begins to fail. If the socket breaks patients often notice an immediate increase in pain with shoulder use.
It stands to reason that younger and more active patients are more likely to experience socket wear in the course of their life as the plastic is exposed to a longer period of use. In addition patients who remain physically active often place higher demands on the shoulder. As more people continue to engage in sports and other demanding recreational activities into their 60’s 70’s and 80’s shoulder replacements are being asked to tolerate more wear and tear – often the same level of use that may have predisposed the shoulder to develop arthritis in the first place.
Younger patients and those who intend to return to a high level of physical activity are at risk of developing socket failure after total shoulder arthroplasty. In certain cases this can occur within the first several years after surgery. When failure occurs additional surgery is usually required to remove the damaged socket. If the bone underneath the socket has also been damaged by the wear and loosening process it may be impossible to replace the socket. In this case the success of revision surgery is less predictable.
Effectiveness
Non-prosthetic glenoid arthroplasty addresses the risk of socket failure in younger and physically demanding patients. Because no plastic is inserted into the joint there are no problems related to artificial socket wear loosening and breaking. In the hands of experienced surgeons this procedure has proven durable in terms of allowing patients to return to their expected level of activity. Some patients who have undergone this procedure have returned to weightlifting water-skiing golf and landscaping. As long as the shoulder is cared for properly and subsequent injuries are avoided the benefit can last for decades.
Shoulder replacement surgery is most effective when the patients are well motivated and follow a simple exercise program after surgery. Thus the patient's motivation and dedication are important elements of the partnership. Especially after non-prosthetic glenoid arthroplasty the need for patience is essential during the early phase of the rehabilitation while the shaped glenoid surface is healing.
Urgency
Shoulder hemiarthroplasty with non-prosthetic glenoid arthroplasty is an elective procedure that can be scheduled when circumstances are optimal for the patient. It is not an urgent procedure. The patient has plenty of time to become informed and to select and experienced surgeon.
Factors that the patient should consider in choosing the optimal time include the following:
- The arthritis has become sufficiently disabling to impair the performance of daily activities. Patients who are still able to sleep comfortably and manage daily activities may consider waiting.
- A planned period of time can be specifically dedicated to the recovery and rehabilitation process that will not interfere with other scheduled events.
- Overall health and nutritional status are optimal and will not limit the ability to comply with the performance of rehabilitation.
- Motivation and readiness to undertake the process of surgery recovery and rehabilitation is a priority.
Risks
The risks of shoulder hemiarthroplasty with non-prosthetic glenoid arthroplasty include but are not limited to the following: infection injury to nerves and blood vessels fracture stiffness or instability of the joint failure of the rotator cuff pain and the need for additional surgeries. There are also risks to anesthesia and blood transfusion (although transfusions are not always necessary). Furthermore it is possible that the joint will remain or become painful without plastic resurfacing of the glenoid. In such a case it may be necessary to revise the hemiarthroplasty to a total shoulder arthroplasty.
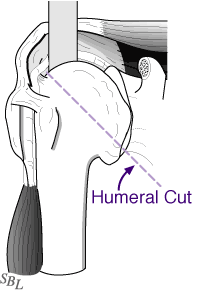
the amount of the damaged ball that is removed.
An experienced shoulder joint replacement team will use special techniques to minimize these risks but cannot totally eliminate them.
Managing risk
Many of the risks of this surgery can be effectively managed if they are promptly identified and treated. Infections may require a "wash out" in the operating room; occasionally removal of the artificial components is necessary. Blood vessel or nerve injury may require repair. Fracture may require surgical fixation. Stiffness or instability may require exercises or additional surgery. If the patient has questions or concerns about the course after surgery the surgeon should be informed as soon as possible.
Preparation
Shoulder hemiarthroplasty with non-prosthetic glenoid arthroplasty is considered for young and physically active individuals in whom arthritis interferes with shoulder function.
The success of surgery depends on a partnership between the patient and the experienced shoulder surgeon. Patients should optimize their health so that they will be in the best possible condition for this procedure. Smoking should be stopped a month before surgery and not resumed for at least three months afterwards. Any heart lung kidney bladder tooth or gum problems should be managed before surgery. Any infection may be a reason to delay the operation. The shoulder surgeon needs to be aware of all health issues including allergies and the non-prescription and prescription medications being taken. Some of these may need to be modified or stopped. For instance aspirin and anti-inflammatory medication may affect the way the blood clots. Since blood transfusion may be necessary patients may choose to have a blood bank draw and store their own blood.
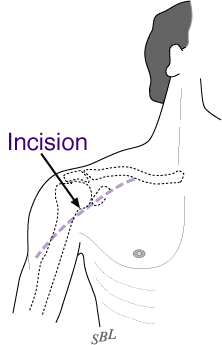
Figure 8 shows the incision used for a shoulder replacement. This area of skin must be clean and free from sores and scratches.
Before surgery patients should consider the limitations alternatives and risks of surgery. Patients should also recognize that the result of surgery depends in large part on their efforts in rehabilitation after surgery.
The patient needs to plan on being less functional than usual for six to twelve weeks after the procedure. Driving shopping and performing usual work or chores may be difficult during this time. Plans for necessary assistance need to be made before surgery. For individuals who live alone or those without readily available help arrangements for home help should be made well in advance.
Timing
Shoulder hemiarthroplasty with non-prosthetic glenoid arthroplasty can be delayed until the time that is best for the patient's overall well being. However in cases of rheumatoid or other types of inflammatory arthritis excessive delays can result in the loss of bone and tendon tissue. These losses can compromise the quality of the surgery and its result.
Costs
The surgeon's office should provide a reasonable estimate of:
- the surgeon's fee and
- the hospital fee.
Surgical team
Shoulder hemiarthroplasty with non-prosthetic glenoid arthroplasty is a technically demanding procedure that should be performed by an experienced surgeon in a medical center accustomed to performing shoulder joint replacements at least several times a month. Patients should inquire as to the number of shoulder replacement procedures that the surgeon performs each year and the number of these procedures performed in the medical center each year.
Finding an experienced surgeon
Because only a few thousand shoulder replacement procedures are performed in the United States each year it is unlikely that every community has an experienced shoulder arthroplasty surgeon who performs many of these procedures each year. The number of surgeons performing non-prosthetic glenoid arthroplasty as described here is small.
Facilities
Shoulder replacement arthroplasty is usually performed in a major medical center that performs these procedures on a regular basis. These centers have surgical teams and facilities specially designed for this type of surgery. They also have nurses and therapists who are accustomed to assisting patients in their recover from shoulder replacement surgery.
Technical details
Shoulder hemiarthroplasty with non-prosthetic glenoid arthroplasty is a highly technical procedure; each step plays a critical role in the outcome.
After the anesthetic has been administered and the shoulder is prepared an incision is made across the front of the shoulder from the middle of the collarbone to the middle of the arm bone as shown in Figure 10. This incision allows access to the joint without damaging the important deltoid or pectoralis muscles that are responsible for a significant portion of the shoulder's power.
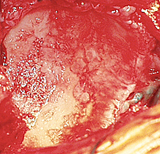
The muscles and other tissues near the shoulder are mobilized by removing any scar tissue that may restrict their motion. The tendon of the subscapularis muscle is cut to gain access to the joint and released circumferentially (a 360-degree release) to restore its length and mobility. Figure 11 shows where the arthritic humeral head (ball of the joint) is removed. The bone spurs are removed to prepare the bone for the humeral prosthesis.
The humeral implant is chosen by trialing different sizes and selecting the one that best matches the patient's anatomy and best restores the muscle balance in the joint without making the joint too tight or too loose. The arthritic glenoid is then refinished using a special spherical reamer. This reaming process corrects the shape and orientation of the socket both of which are affected by shoulder arthritis. The curvature of the reamer nearly matches that of the humeral ball and this matching surface allows smooth and stable rotation of the ball in the socket. Figure 12 shows the arthritic glenoid and figure 13 shows the glenoid after it has been reamed.
In this procedure the glenoid shape and orientation are corrected but a glenoid prosthesis is not inserted. Once the reaming process is completed the final humeral component is inserted. The subscapularis tendon is then carefully repaired and closure of the muscle and skin layers completes the procedure. A drain is placed which is removed on the second morning after surgery. This prevents blood from collecting in the wound.
Anesthetic
Shoulder replacement surgery may be performed under a general anesthetic or under a brachial plexus nerve block. A brachial plexus block can provide anesthesia for several hours after the surgery. The patient may wish to discuss their preferences with the anesthesiologist before surgery.
Length of non-prosthetic glenoid arthroplasty
The procedure usually takes approximately two hours however the preoperative preparation and the postoperative recovery may add several hours to this time. Patients often spend two hours in the recovery room and two to four days in the hospital after surgery.
Pain and pain management
After the non-prosthetic glenoid arthroplasty the reamed glenoid surface must heal. This process may require up to a year to complete. Thus recovery of comfort and function after shoulder hemiarthroplasty with non-prosthetic glenoid arthroplasty continues for the first year after surgery. The rehabilitation is carried out largely by the patient under the supervision of the surgeon.
Shoulder replacement of this type is a major surgical procedure that involves cutting of skin tendons and bone. The pain from this surgery is managed by the anesthetic and by pain medications. Immediately after surgery strong medications (such as morphine or Demerol) are often given by injection. Within a day or so oral pain medications (such as hydrocodone or Tylenol with codeine) are usually sufficient.
Because a plastic socket is not inserted when a non-prosthetic glenoid arthroplasty is performed there may be some initial added discomfort from the metal ball articulating with the bone. When the glenoid is reamed small fractures in the surface bone are intentionally created. These tiny surface fractures initiate a healing response that improves the smoothness of the socket and may help distribute force from the arm to the body. This healing process may make the first 6 weeks more uncomfortable than a total shoulder replacement surgery. This discomfort should be only temporary and as the healing process completes comfort levels are expected to approach that of total shoulder arthroplasty.
Use of medications
Initially pain medication is usually administered intravenously or intramuscularly. Sometimes patient controlled analgesia (PCA) is used to allow the patient to administer the medication as it is needed. Hydrocodone or Tylenol with codeine are taken by mouth. Intravenous pain medications are usually needed only for the first day or two after the procedure. Oral pain medications are usually needed only for the first two weeks after the procedure.
Effectiveness of medications
Pain medications can be very powerful and effective. Their proper use lies in the balancing of their pain relieving effect and their other less desirable effects. Good pain control is an important part of the postoperative management.
Important side effects
Pain medications can cause drowsiness slowness of breathing difficulties in emptying the bladder and bowel nausea vomiting and allergic reactions. Patients who have taken substantial narcotic medications in the recent past may find that usual doses of pain medication are less effective. For some patients balancing the benefit and the side effects of pain medication is challenging. Patients should notify their surgeon if they have had previous difficulties with pain medication or pain control.
Hospital stay
After surgery the patient spends an hour or so in the recovery room and is then transferred to a private room. The drain is usually removed on the second day after surgery. Bandages cover the incision. They are usually changed the second day after surgery.
Patients are discharged as soon as the incision is dry the shoulder is comfortable with oral pain medications the patient can perform the range of motion exercises and the home support systems for the patient are in place. Discharge is usually on the third or fourth day after surgery.

Recovery and rehabilitation in the hospital
Early motion after shoulder hemiarthroplasty with non-prosthetic glenoid arthroplasty helps achieve the best possible shoulder function. Arthritic shoulders are stiff. Early motion is facilitated by the complete surgical release of the tight tissues so that after surgery the patient has only to maintain the range of motion achieved at the operation. However after surgery scar tissue will tend to recur and limit movement unless motion is started immediately. Early motion also facilitates healing of the glenoid bone and ensures that a smooth bony surface will form to articulate with the metal ball.
A continuous passive motion (CPM) machine is often used to gently move the shoulder in the recovery room immediately after surgery. The CPM machine shown in figure 11 is used for the first few days after surgery whenever the patient is in bed.
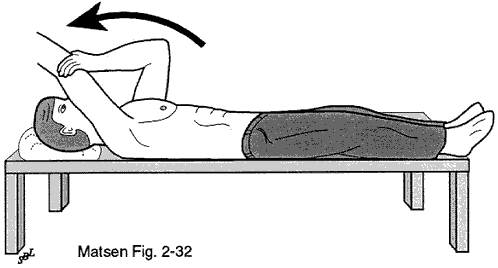
During the hospitalization the patient learns a simple rehabilitation program that will be used for maintaining the range of motion at home after discharge. Figures 12 shows the exercise used to maintain elevation and rotation of the arm. On the day of surgery or on the day after the physical therapist teaches the patient gentle range of motion exercises. The patient is usually shown how to stretch the shoulder forward and out to the side preventing stiffness and adhesions.
Walking and use of the arm for gentle activities are encouraged soon after surgery.
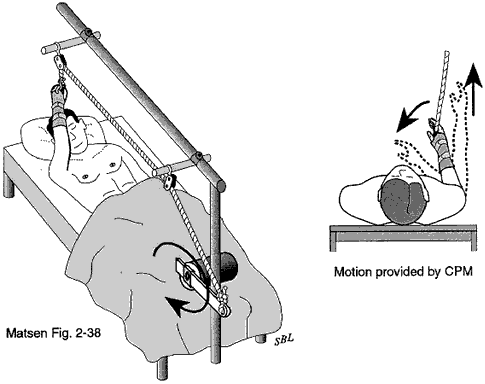
motion machine
Hospital discharge
At the time of discharge the patient should be relatively comfortable on oral medications should have a dry incision should understand their exercises and should feel comfortable with the plans for managing the shoulder. For the first month or so after this procedure the operated arm may be less useful than it was immediately beforehand.
The specific limitations can be specified only by the surgeon who performed the procedure. It is important that the repaired tendons not be challenged until they have had a chance to heal. Usually the patient is asked to lift nothing heavier than a cup of coffee for six weeks after the surgery.
Management of these limitations requires advance planning to accomplish the activities of daily living during the period of recovery.
Convalescent assistance
Patients usually require some assistance with self-care activities of daily living shopping and driving for approximately six weeks after surgery. Patients usually go home after this surgery especially if there are people at home who can provide the necessary assistance or if such assistance can be arranged through an agency. In the absence of home support a convalescent facility may provide a safe environment for recovery.
Recovery of comfort and function after shoulder hemiarthroplasty with non-prosthetic glenoid arthroplasty continues for many months after the surgery. Improvement in some activities may be evident as early as six weeks. With persistent effort patients make progress for as long as a year after surgery.
Physical therapy
Early motion after shoulder hemiarthroplasty with non-prosthetic glenoid arthroplasty is critical for achieving optimal shoulder function.
Arthritic shoulders are stiff. Although a major goal of the surgery is to relieve this stiffness by release of scar tissue it may recur during the recovery process if range of motion exercises are not instituted immediately. For the first 6 weeks of the recovery phase the focus of rehabilitation is on maintaining the motion that was recovered at surgery. Strengthening exercises are avoided during the first 6 weeks so as not to stress the tendon repair before it heals back to the bone. Later on once the shoulder is comfortable and flexible strengthening exercises and additional activities are started.
Rehabilitation options
It is often most effective for the patient to carry out their own exercises so that they are done frequently effectively and comfortably. Usually a physical therapist or the surgeon instructs the patient in the exercise program and advances it at a rate that is comfortable for the patient.
Structured outpatient physical therapy is usually not necessary during the initial phase of recovery as the gentle stretching exercises are more effectively performed by the patient. When strengthening exercises are added to the program--often at around 6 weeks--outpatient physical therapy for rotator cuff strengthening may be beneficial. However motivated patients may also perform these exercises at home with equal effectiveness. Occasional visits to the surgeon or therapist may be useful to check the progress and to review the program.
Usual response
Patients are almost always satisfied with the increases in range of motion comfort and function that they achieve with the exercise program. If the exercises are uncomfortable difficult or painful the patient should contact the therapist or surgeon promptly.
Risks
This is a safe rehabilitation program with little risk.
Duration of rehabilitation
Once the range of motion and strength goals are achieved the exercise program can be cut back to a minimal level. However gentle stretching is recommended on an ongoing basis. In addition a maintenance program to keep the rotator cuff muscles strong and healthy will ensure proper function of the artificial joint and may help prolong its benefit.
Returning to ordinary daily activities
In general patients are able to perform gentle activities of daily living using the operated arm from two to six weeks after surgery. Walking is strongly encouraged. Driving should wait until the patient can perform the necessary functions comfortably and confidently. Recovery of driving ability may take six weeks if the surgery has been performed on the right shoulder because of the increased demands on the right shoulder for shifting gears.
With the consent of their surgeon patients can often return to activities such as swimming golf and tennis at six months after their surgery.
Long-term patient limitations
One of the primary goals of shoulder hemiarthroplasty with non-prosthetic glenoid arthroplasty is to allow physically demanding individuals to return to activities that would otherwise have been prohibited with the implantation of a plastic socket. While there are no strict limitations on participation those activities that involve impact (chopping wood contact sports) and those that involve heavy loads (weightlifting) may predispose the rotator cuff tendons to injury and tear. Thus patients should take caution in these types of activities to minimize the risk of damage to the operated shoulder.
Costs
The surgeon and therapist should provide the information on the usual cost of the rehabilitation program. The program is quite cost-effective because it is based heavily on home exercises.
Summary of non-prosthetic glenoid arthroplasty for arthritis of the shoulder
Shoulder hemiarthroplasty with non-prosthetic glenoid arthroplasty helps restore comfort and function to shoulders damaged by degenerative joint disease and osteoarthritis. This procedure provides an approach to treating arthritis in young and physically demanding patients whose arthritis has advanced to the point of surgical treatment. By reshaping reorienting and smoothing the bony socket this procedure removes the risks associated with wear loosening and fracture of the plastic socket.
In the hands of an experienced surgeon shoulder hemiarthroplasty with non-prosthetic glenoid arthroplasty can be an effective method for treating shoulders with damaged joint surfaces in a healthy and motivated patient. Pre-planning and persistent rehabilitation efforts will help assure the best possible result for the patient.
